I am often asked to review ECG reports on cardiac pacing.
This one was reported as intermittent failure of ventricular capture.
What do you think? I am showing the rhythm strips, which are easier to interpret.
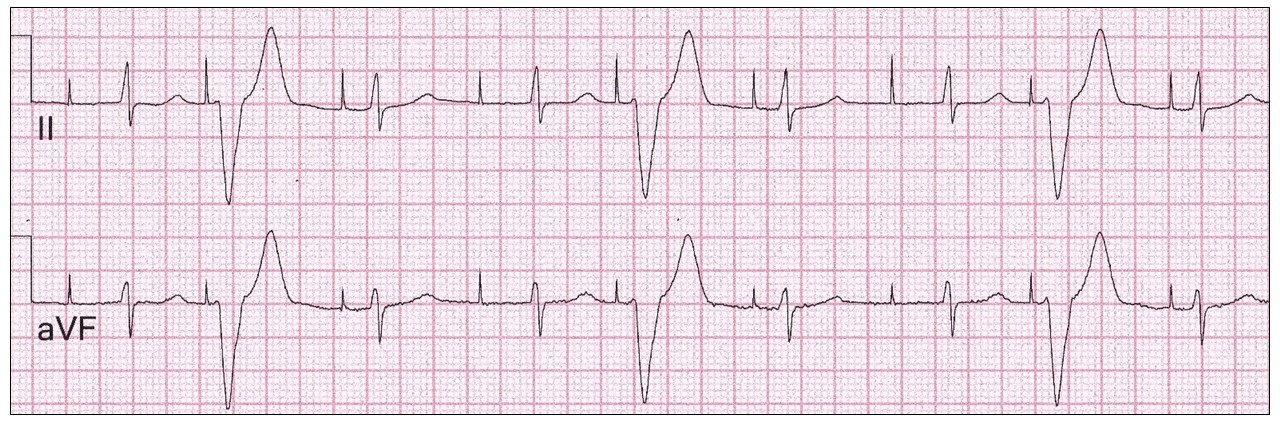
I felt this was atrial pacing. Anyone agree?
In order to interpret the tracing, we need to revisit atrial pacing.
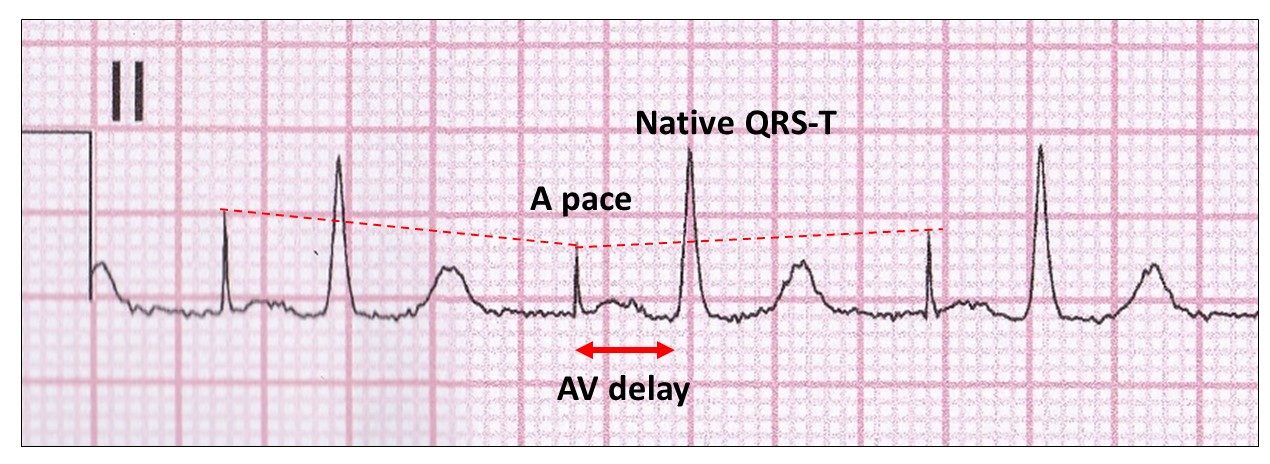
This is an ECG of single chamber atrial pacing (AAI). Following the atrial stimulus artefact, there is atrial depolarization (A pace) followed by an atrioventricular delay (AV delay with conduction to the ventricle (native QRS-T).
Note the stimulus artefact varies in height due to respiration (red stippled line).
Usually the bipolar stimulus artefact is very small:
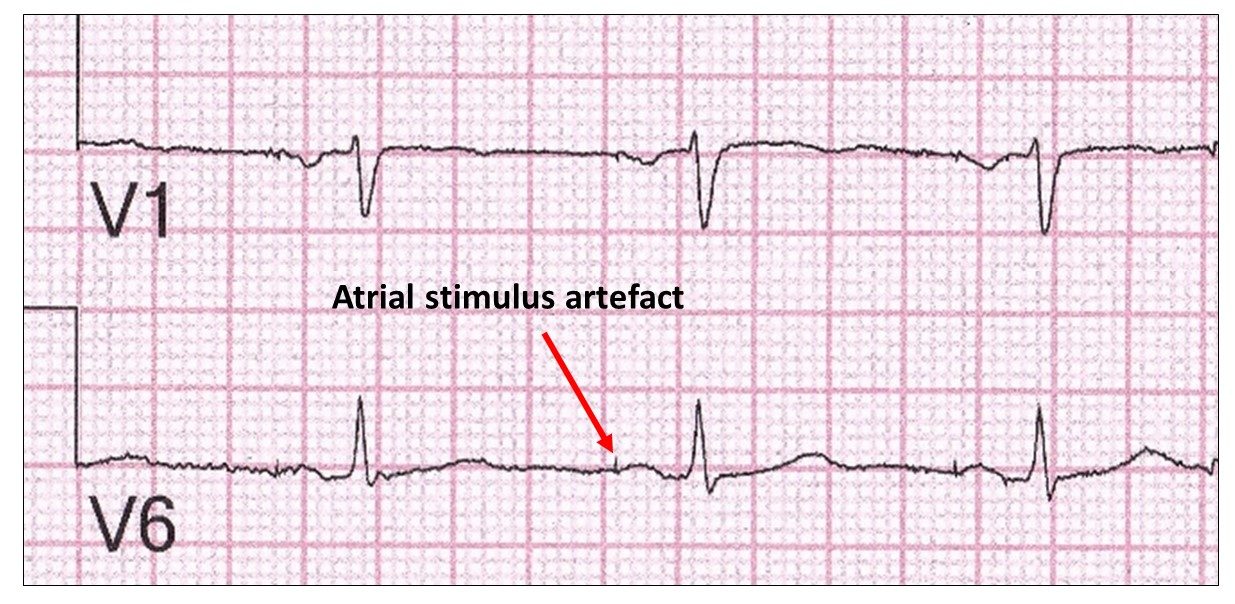
And the P wave difficult to see:
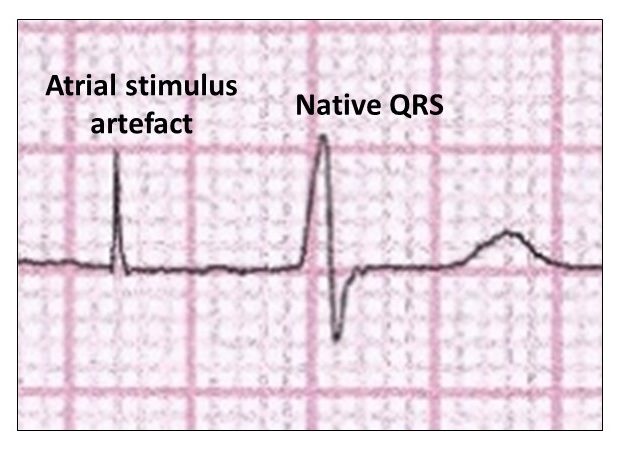
The clue with atrial pacing is AV conduction.
If the stimulus lies within the P wave, think of AAT pacing:
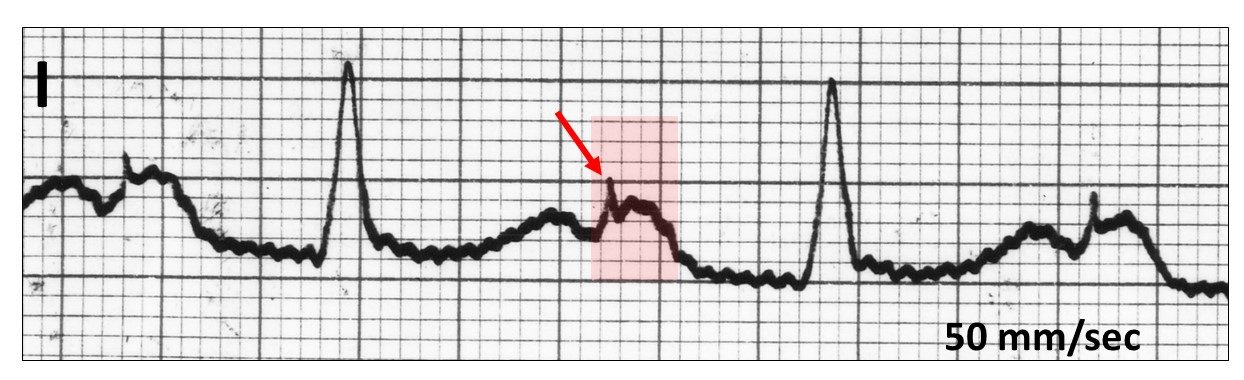
Upon atrial sensing, a full stimulus artefact (red arrow) is delivered into the P wave (red highlight).
The paced P wave may be biphasic with severe atrial disease (red highlight).
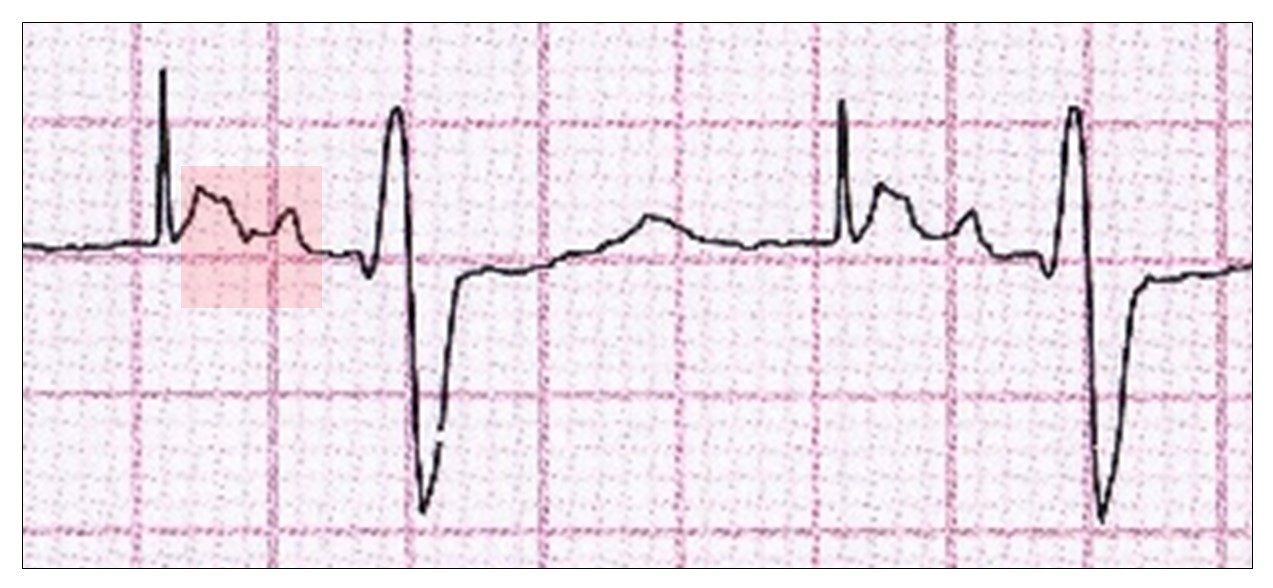 A delay between the stimulus artefact and atrial depolarization (P wave) is referred to as atrial latency or first-degree pacemaker atrial block.
A delay between the stimulus artefact and atrial depolarization (P wave) is referred to as atrial latency or first-degree pacemaker atrial block.
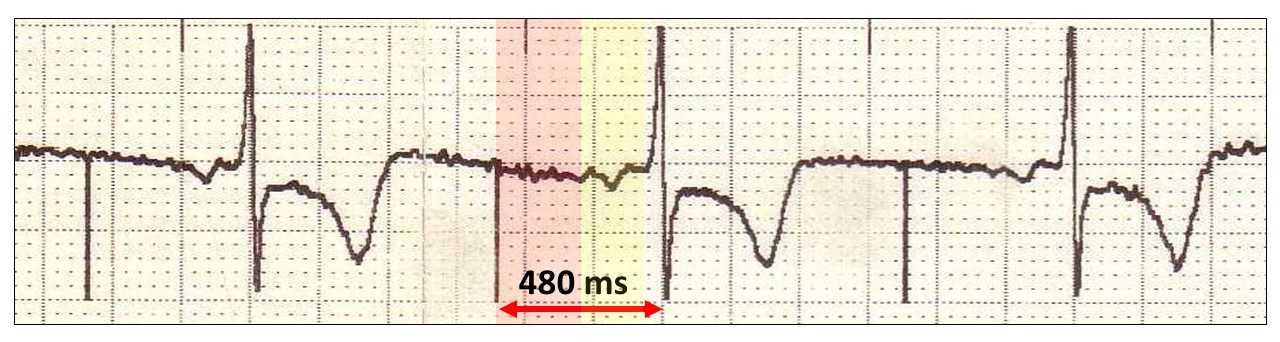
The latency period (red highlight) is followed by the P wave (yellow highlight) resulting in a very long AV delay and reflects serious atrial disease.
A prolonged AV delay will also occur with AV conduction disease, which is common in the elderly.
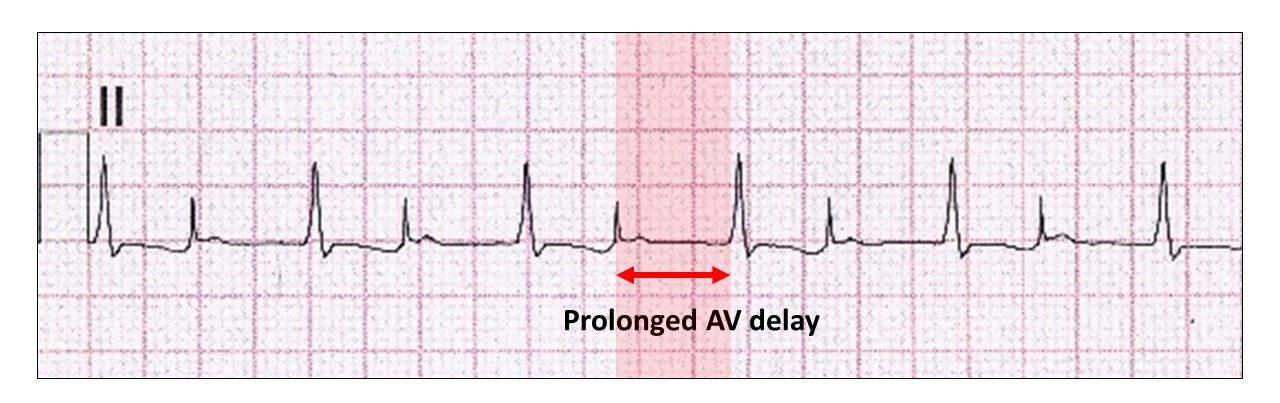
Single chamber AAI pacing is rarely used for a number of reasons, the most quoted being progression to higher degrees of AV block.
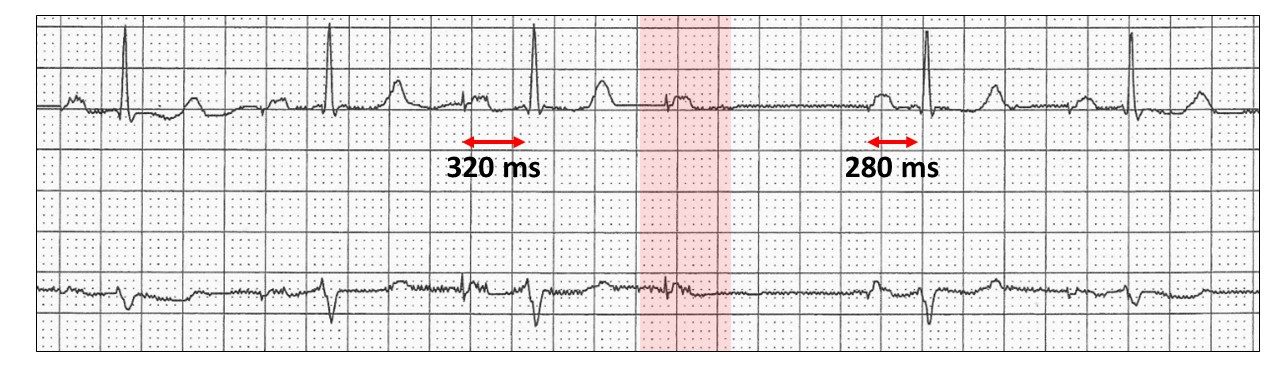
Although this looks sinister, remember most of these patients had single chamber AAI pacemakers implanted for sinus node disease and the pause may be innocent nocturnal Wenckebach AV block.
One of the poorly understood ECG features of AAI pacing are ventricular ectopics:
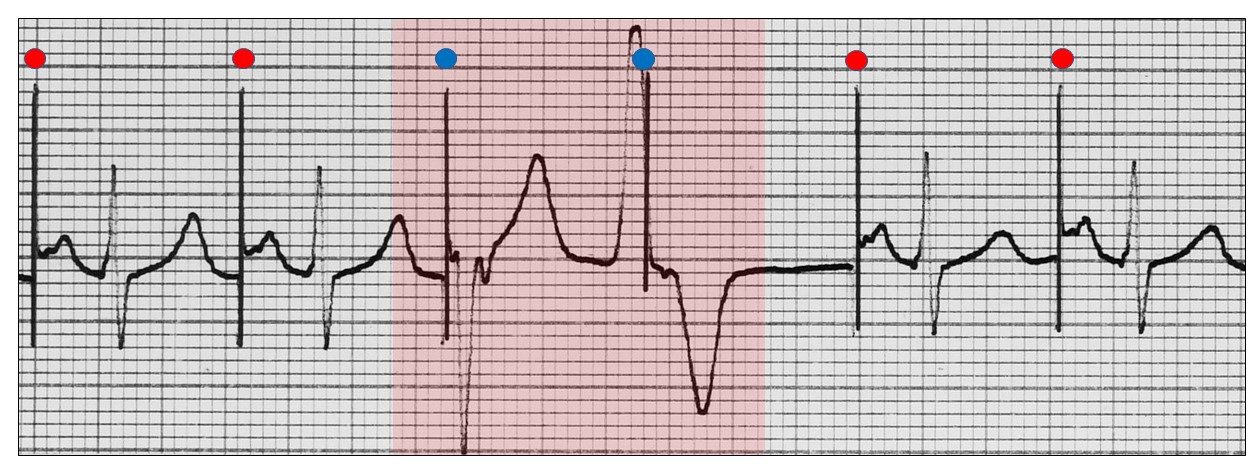
There appears to be under-sensing. Remember the atrial channel cannot sense electrical activity in the ventricle unless it is far field or retrograde conduction. In this example, there is a ventricular couplet (red highlight). The atrial stimulus artefacts (red dots) continue unabated through the ectopics, and atrial depolarization is concealed and does not conduct to a refractory conducting system (blue dots).
Remember this is normal atrial pacemaker function!
Because of the timing the ventricular ectopic often appears late (end diastolic) resulting in a confusing appearance, which may mimic ventricular pacing.
These features are summarized:
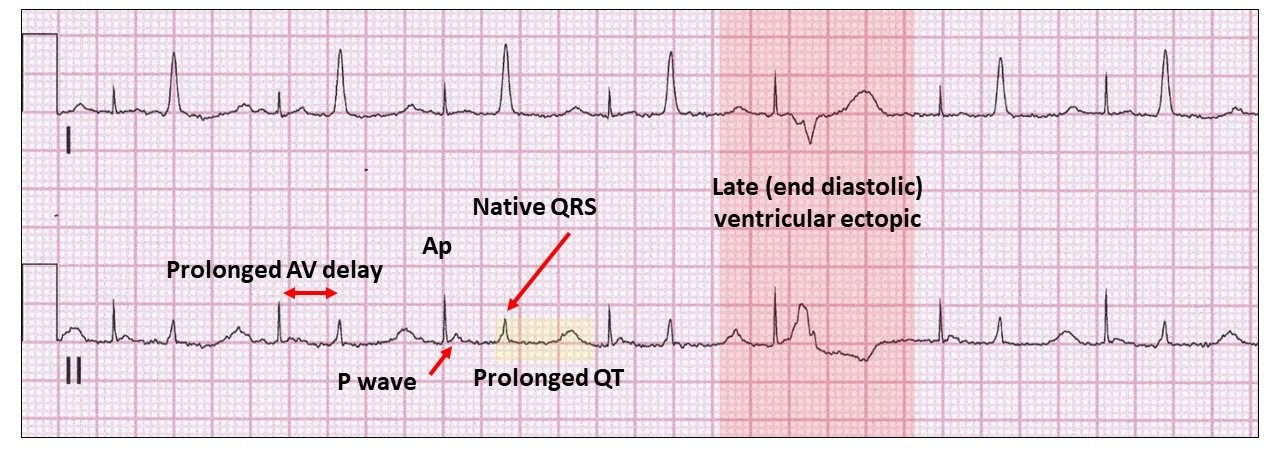
There is a prolonged AV delay resulting in the ventricular ectopic being end diastolic (red highlight). There is also a prolonged QT interval or rather a prolonged ST interval (yellow highlight). Think of the possible causes.
These appearances are further complicated with an increase in the atrial pacing rate (AAIR).
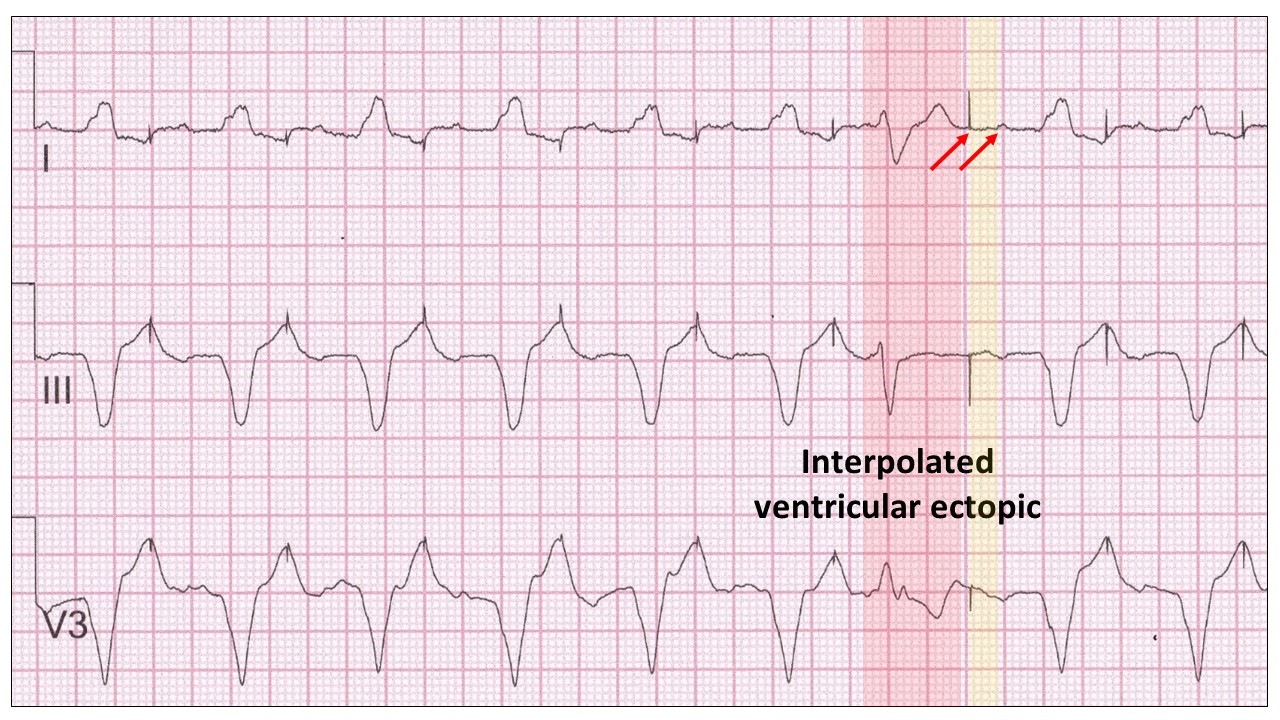
Now the atrial stimulus artefact falls into the T wave of the previous broad QRST and may result in the atria contracting against closed AV valves. These patients have marked symptoms with mild exertion, which would be corrected by shortening the AV delay with ventricular pacing.
The end diastolic ventricular ectopic (red highlight) is actually interpolated, although the prolonged AV delay gives the appearance of a compensatory pause.
This pseudo-compensatory pause allows us to inspect the AV delay which shows atrial latency meaning the atrium would contact well after the stimulus artefact (red arrows and yellow highlight).
The wide paced QRS and the AV latency suggests poor cardiac function.
Let us return to our original ECG:
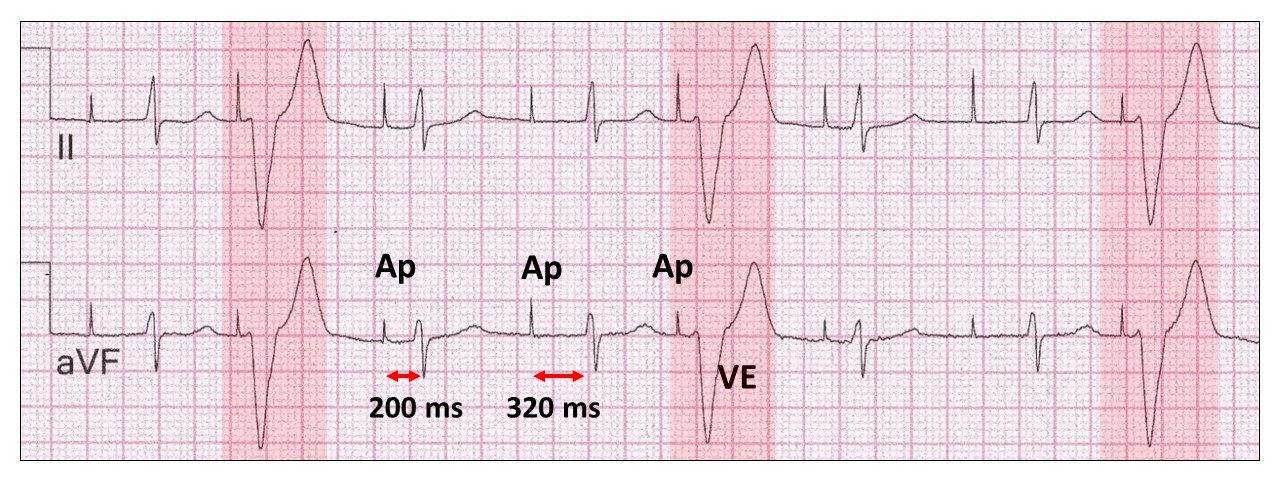 Atrial pacing (Ap), very poor P wave and Wenckebach AV conduction, but no dropped beats because of end diastolic ventricular trigeminy (VE, red highlight).
Atrial pacing (Ap), very poor P wave and Wenckebach AV conduction, but no dropped beats because of end diastolic ventricular trigeminy (VE, red highlight).
Remember, it’s all in the timing
Harry Mond






 A delay between the stimulus artefact and atrial depolarization (P wave) is referred to as atrial latency or first-degree pacemaker atrial block.
A delay between the stimulus artefact and atrial depolarization (P wave) is referred to as atrial latency or first-degree pacemaker atrial block.





 Atrial pacing (Ap), very poor P wave and Wenckebach AV conduction, but no dropped beats because of end diastolic ventricular trigeminy (VE, red highlight).
Atrial pacing (Ap), very poor P wave and Wenckebach AV conduction, but no dropped beats because of end diastolic ventricular trigeminy (VE, red highlight).